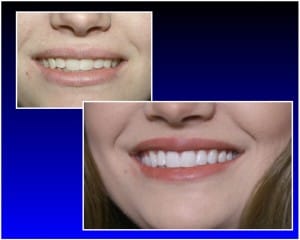
 One of the first pieces of advice professionals give when treating people with low self-esteem is: “Smile!” Smiling releases endorphins which make you feel better about everything, including yourself and your circumstances. But what if you don’t like your smile? What if you have problems with your teeth and for whatever reason, have never had them corrected? What if you have a very good reason for not smiling? Is there no hope for your self-esteem? Obviously, there is, or we wouldn’t be writing this article! Below are the most common complaints we hear from patients about their smile, and what you can do to fix them. “I’m embarrassed by how crooked my teeth are.” Many people have grown into adulthood with crowded teeth and misaligned smiles. Unfortunately, this can lead to issues with the desire to display your pearly whites in public. While many are aware that orthodontics (braces) is an option, most don’t want to go through two to three years of treatment or be called “metal mouth.” But did you know that we now have options available that take much less time than traditional orthodontics, and some that would not be noticeable at all? Invisalign® is a product that can be used in many adult cases to give the effects of traditional orthodontics. The difference is that the appliances are clear and virtually undetectable to others. Many famous actors, news casters, and other TV personalities have worn aligners on air and no one noticed! The procedure for Invisalign is that plastic “aligners” are made for your teeth that will gently and gradually move them into proper alignment. Your teeth will become a little sore, just as with traditional orthodontics, but it’s not anything you can’t bear. In a few months, or some cases weeks, your teeth are straight! Another option for correcting tooth alignment is veneers. Dr. Moorhead can remove a layer of your tooth structure and replace it in a way that straightens the alignment of your overall smile. Veneers are porcelain or composite (a mixture of about 75% glass dust and 25% acrylic) “shells” that are chemically bonded to the surface of a tooth to repair it or just change the tooth’s appearance, and are vastly considered the fastest way to straighten teeth. “I often have bad breath. I don’t know what to do about it, so I just don’t risk it and avoid opening my mouth as much as possible.” While there are many causes of bad breath, the most common is a long hiatus from your dental hygienist! With that said, be sure to tell Dr. Moorhead if you’ve noticed breath problems so that he can help identify the cause professionally and refer you to the appropriate specialist if necessary. When the problem is strictly dental related, there are lots of options, the first being to get regular cleanings. Most adults need regular dental cleanings every 3 to 6 months. Only a dentist or hygienist can determine the proper schedule for you, but they will be glad to do so. Foods such as garlic, onions, and other strong substances contribute to objectionable breath odor. Once the food is absorbed into the bloodstream, it is transferred to the lungs, where it is expelled when you talk. Brushing, flossing and using mouthwash will mask the odor temporarily, but odors will continue until the body eliminates the food. Dieters sometimes develop unpleasant breath due to infrequent eating. Drinking water to keep your mouth moist will help with this problem. Brushing and flossing daily helps to eliminate particles of food that can remain in the mouth, collecting bacteria, and causing bad breath. Food that collects between the teeth, on the tongue and around the gums can rot, leaving an unpleasant odor. Since saliva cleanses the mouth and removes particles that may cause odor, bad breath can also be caused by a lack of saliva, or “dry mouth.” The clinical term for dry mouth is xerostomia, which occurs when the flow of saliva decreases. This problem seems to develop most often in older adults. Dry mouth may be caused by various medications, salivary gland problems or continuously breathing through the mouth. If you suffer from dry mouth, Dr. Moorhead can prescribe artificial saliva. Other suggestions include using sugarless candy and increasing your fluid intake. Tobacco products cause bad breath. We’ve noticed that after awhile, a smoker’s breath will have a “stale” smell to it. If you use tobacco, consider quitting and ask your dentist for tips on kicking the habit. Dr. Moorhead has special training in this area and can offer everything from advice, to prescriptions as needed. Mouthwashes are generally cosmetic and do not have a long-lasting effect on bad breath. If you find yourself constantly using a breath freshener to hide unpleasant mouth odor, see your dentist. He or she may recommend using a special antimicrobial mouth rinse. Bad breath may be the sign of a medical disorder, such as a local infection in the respiratory tract, chronic sinusitis, postnasal drip, chronic bronchitis, diabetes, gastrointestinal disturbance, liver or kidney ailment. If your dentist determines that your mouth is healthy, you may be referred to your family doctor or a specialist to determine the cause of your bad breath. Learning the cause and that there is hope will do wonders for your self-esteem. “I have these spots on my teeth that have been there since I was a child. I just assume that since they’ve always been there, there’s nothing I can do.” Oh, but there are plenty of things Dr. Moorhead can do! Sometimes these spots are a decalcification of the tooth enamel that can be treated with a simple fluoride solution, or a new material called MI Paste. Special trays are made for your mouth, and then the fluoride solution or MI paste is placed in them so that it can be held against your teeth for several minutes. The length and number of treatments just depends on the severity of the problem. There is also a process called micro-abrasion. Dr. Moorhead can use a special substance and appliance to gently, but effectively, remove the trouble spots to give your teeth a smoother, more consistent appearance. “My teeth have an overall gray (or beige) appearance. I’ve tried whitening, but it doesn’t work. I just don’t think a white smile is ‘in the cards’ for me.” What you probably have is the result of tetracycline treatment, or excessive fluoride that you encountered as a young child while your teeth were forming. It’s true that even some professional whitening systems are not effective against this condition, but we do have other methods of treating this problem. Some dentists use a resin material to bond over stained teeth. This method is quick and easy, but the material does stain and chip over time. The best method, and what we use most in our office, is porcelain veneers. Veneers are like shells for your teeth, and are much more durable than bonding. Porcelain is more translucent than resin, meaning that it is more like a natural, healthy-white tooth, giving you a more natural-looking, beautiful appearance. “Too much of my gums show when I smile.” Believe it or not, there is an answer for this, too! Crown lengthening is a procedure where the gum line is altered in order to expose more of the tooth structure, and less of your gums. This operation is sometimes necessary in order to properly restore a tooth, but it can be purely cosmetic also to give the result of a better smile line. Some general dentists are performing this procedure in their own offices, but some cases still require referral to a specialist. Either way, the investment is well worth it. If you just don’t feel like smiling, do it anyway! Studies show that the act of smiling can actually boost confidence, and everyone knows that a confident person smiles. Try it; you’ll be glad you did! Most importantly, whatever the reason for your not liking your smile, please discuss it with us. We’re professionals and take your trust in us very seriously. We never laugh, joke, or kid around when it comes to something as important as your smile, or your self-esteem.
1 Comment
Did you know that the #1 tool most people use for cleaning bacteria from their teeth, gums, and mouth, already contains millions, possibly trillions, of bacteria? If you leave your toothbrush in the bathroom and never disinfect it, you’d better read this article.
In his book, Why Your Toothbrush May Be Killing You Slowly, James Song, a biochemist from Wisconsin University, suggests that a range of serious health problems, including heart disease, stroke, arthritis and chronic infections, could be linked to unhygienic toothbrushes. Further research by Manchester University found that the average toothbrush contained around ten million germs, including a high percentage of potentially fatal bacteria such as staphylococci, streptococcus, E. coli and candida. Other studies have shown that over time, a single toothbrush can be the breeding ground for trillions of bacteria specimen. There are many ways these bacteria latch on to toothbrushes: Use from an infected user, spray from a flushing toilet, a damp environment that allows the bacteria to breed and grow, and just a general lack of oversight. Think about it for a moment; would you leave your eating utensils in the bathroom, use them over and over again, and never wash them? As bad as it sounds, overcoming this potential time bomb is not complicated. Below are Dr. Moorhead’s 5 simple tips to keep your toothbrush bacteria free.
If you have any questions or would like further advice on disinfecting your toothbrush, please contact us using one of the methods below, or ask us at your next appointment.  One of the most commonly misunderstand concepts of good oral hygiene is that one should avoid sugar at all costs. Why? Well, sugar causes tooth decay. Yes, that is true, but did you know that most diet sodas are one-tenth as strong as battery acid? How good do you think that is for your teeth? You guessed it, not at all! Furthermore, once tooth enamel has become weakened by sugar and acid, we see a lot of damage caused by hard candy or other tough foods. Throw in the double-whammy of the fact that most people with a diet high in sugar and diet sodas are not getting enough of the right nutrients, and you’ve created an environment that will very likely lead to cavities. Here’s what happens: You get up in the morning and brush your teeth before leaving for work. On the way to work, you stop for a cup of coffee, maybe a muffin. If you’re like most people, you don’t have or take the time to brush your teeth immediately. What’s happening in your mouth is that that food leaves a film that becomes bacterial in nature, also known as plaque. The next thing you know it’s time for lunch. You grab a sandwich, maybe some chips, and a diet soda. When the plaque that has been building up all morning comes into contact with these new sugars, (from the sandwich and chips), acid is produced which attacks the enamel on your teeth. This process takes about 20 minutes, and, if nothing is done, the attack can eventually result in tooth decay. The more often you eat and the longer foods are in your mouth, the more damage occurs. Now imagine that you skip the step of the bacteria and sugar and go straight to the acid attacking the enamel. That’s what you’re doing when you drink diet sodas. Even if no plaque is present, for each sip of diet soda, the acid gets to eat on your enamel for 20 minutes. Getting the picture? So what’s the answer? Here are 8 suggestions for good dental-diet habits.
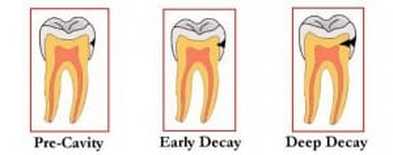
If you have further questions about how your diet affects your dental health, please contact us at Flemingsburg Dental Care. 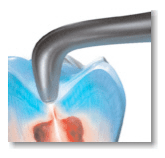 Ever wonder how dentists know whether there is a cavity in a tooth? We use x-rays to look for cavities in-between teeth, but how does a dentist know if there’s decay in the grooves of your teeth? In the past, the dental profession has traditionally used a dental explorer to feel for soft spots in the grooves of teeth. Unfortunately, there was often some guesswork involved. Before fluoride was added to our community water supplies to help prevent cavities, decay would often be a large hole and easy to spot. Since fluoride has been used, dental decay in the grooves of teeth now is very narrow and more difficult to diagnose. A newer technology that is now available in our office is a laser device called a Diagnodent. This device shines a laser light into the grooves of your tooth, and a numeric value is displayed that indicates how much decay is present. It’s completely painless, and even very small cavities can be detected at their earliest stage, so that decay can be caught before more tooth structure is damaged. Cavities can start in the grooves of teeth even before a child’s tooth fully appears. In almost 90% of molar teeth, the grooves aren’t formed completely. A dental sealant can be placed soon after the tooth erupts to protect these incompletely formed grooves in the teeth from developing cavities.  In our office, we use the Diagnodent laser to tell us if a sealant can be used. When the Diagnodent’s digital reading displays a reading of 23 or higher, we know there is an actual cavity present that requires a filling. For a reading of 22 or less, we can place a sealant to keep the tooth from getting a cavity in the first place. For more information on the Diagnodent, or to schedule your next appointment, contact us today. You’re seeing commercials on television that talk about a product’s ability to reverse cavities. So can these products really work? And what works best? First a little bit of background. A tooth actually develops a “cavity” when bacteria eats through the outer enamel layer of the tooth and gets into the softer dentin layer that lies below the enamel. In your mouth, these demineralized areas, or “pre-cavities” look like opaque white or brown spots, as shown in the picture below. We’ve known for several years that you can use fluoride to reverse a pre-cavity, but it requires repeated regular applications of fluoride to accomplish this reversal. Two of the best ways to accomplish this are with application of fluoride varnishes or the daily use of custom fluoride trays at home. Fluoride varnish is a highly concentrated temporary dose of fluoride. The varnish holds fluoride close to the tooth surface for a longer period of time than other concentrated fluoride products. The varnish, usually tooth colored, is applied by a dental professional. When the varnish is used repeatedly, it can actually reverse the pre-cavity by remineralizing the tooth. 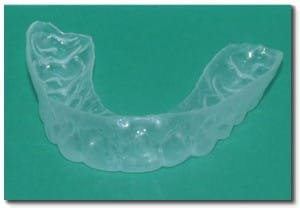 Custom fluoride trays look similar to bleaching trays or whitening trays, but are specifically designed to cover your teeth completely at the gum line. They are fabricated to fit directly over your upper and lower teeth, and are used to hold a few drops of concentrated fluoride on the teeth. For about the cost of having one cavity filled, the custom fluoride trays provide you with a way of doing a professional strength fluoride treatment every day. To use the custom fluoride trays, we recommend the following regimen:
There are some newer products that are even more effective at reversing pre-cavities. A product called MI Paste can reverse the pre-cavities and often reverse the opaque white spot caused by the pre-cavity. MI Paste works by releasing calcium and phosphate ions into your tooth enamel. It can be brushed on, or can be worn in the custom fluoride trays already mentioned. There are many effective tools for fighting cavities before they start. Give us a call today so that we can help give you the smile you want. If you have or might have periodontal disease, also sometimes called “gum and bone” disease, we know that you are at risk for other health problems. For instance, researchers have now shown us that untreated gum and bone disease directly increases your risk for heart disease and strokes. The bacteria under your infected gums release toxins into your bloodstream that ultimately travel to the heart.
According to one theory, when the bacteria travel into the blood stream, the microbes attach to fatty plaque in the blood vessels of the heart. The artery walls thicken with the buildup of fatty proteins, ultimately causing clots to form. When your normal blood flow is restricted by clotting, the heart’s function is impaired, keeping it from taking in oxygen and nutrients as efficiently. As heart function gradually diminishes, a diseased condition eventually develops that can eventually lead to a heart attack. Even the slightest amount of gum inflammation in your mouth causes bacteria to enter the bloodstream that can cause all of these problems. Diabetics are more prone to periodontal disease. If left untreated, gum disease makes it harder for diabetics to control their blood sugar. When gum disease is eliminated, diabetics improve their blood sugar control and make diabetic complications less likely. And with diabetes, it’s kind of a two way street. Periodontal disease makes it harder to control blood sugar levels (making diabetes worse), and diabetic patients have a harder time fighting off infection when it occurs, including periodontal disease. Gastric ulcers are caused by bacteria. When your gums are inflamed, bacteria from the mouth can travel to the stomach and cause ulcers to become active. If you have been treated for ulcers, you should make sure your gums are as inflammation free as possible. Several other health conditions can make you more prone to periodontal disease, including:
If you have conditions that make you more prone to periodontal disease, why not give us a call today? Contact us at 606.845.2273, or toll-free at 888.917.2273. Click here for a special offer for new patients in our practice. Endodontic, or more commonly called “root canal” therapy, is a highly successful procedure – an overall 85% success rate. If the nerve and blood vessels inside your teeth, also known as the “pulp,” become infected, endodontic treatment can be used to save your tooth.
Endodontic procedures are usually needed if deep decay has progressed far enough that it infects the pulp chamber of your tooth, or if the tooth receives a blow or other severe trauma. The question Dr. Moorhead gets asked most about root canal therapy is one you’d probably expect: “Does it hurt?” We’ve all heard the stories told from years ago where someone had a root canal procedure performed and encountered lots of problems. Comedians and late night talk show hosts routinely refer to “root canals” as procedures to be avoided. But endodontic treatment has changed so much with today’s technology that it can’t even be compared to the stories people talk about. Endodontic treatment used to involve two to three appointments, and at the very least, the tooth was very sore. With the techniques we use in our office, at least 98% of endodontic procedures can be completed in just one appointment. Dr Moorhead routinely phones patients at night to make certain that they are doing well after their dental procedures. When hw phones our patients who have had a “root canal” earlier in the day, Dr. Moorhead routinely hear one of two responses – either the tooth feels “great,” or at worst, it’s “just a little tender to bite on.” That's quite a difference from what most patients expected! There are a couple of other things we do at Flemingsburg Dental Care to make certain our patients are comfortable during and after endodontic procedures. When necessary, Dr. Moorhead will prescribe an antibiotic in advance so that there aren’t any problems getting the patient numb. In addition, we routinely recommend that the patient take a non-steroidal anti-inflammatory medication, such as Aleve, one hour before the procedure, and for two to three days after the appointment. For patients who have always had problems getting numb or are highly anxious about their procedure, we use sedation dentistry. If you’ve been putting off root canal therapy, why not give us a call today? Click here for a special offer for new patients in our practice. Many people wonder why it’s necessary to replace missing teeth. Let’s see what happens when a tooth is lost and is not replaced. 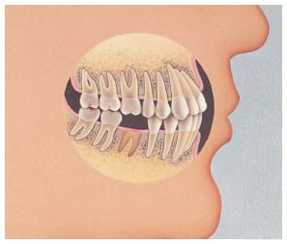 For the sake of our example, we’ll presume you have a missing lower molar, as in the photo here. 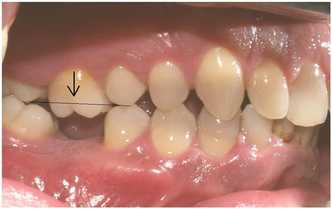 When we’re young and our teeth are erupting, they’re programmed to keep erupting until they meet something. So when you lose a tooth and don’t replace it, the process starts again. The corresponding tooth in your opposite jaw will once again start erupting. Unfortunately, when the shifting occurs, the tooth moves, but the bone that holds in the tooth does not move with it. This results in a loss of bone support for the opposing tooth 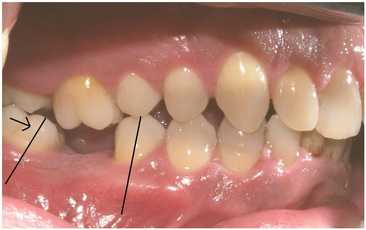 Teeth also literally lean on each other. When you lose a tooth, the tooth immediately behind shifts forward. This throws off your bite and makes you more prone to tooth grinding (“bruxism”) and disorders related to the joint between the upper and lower jaws, the TMJ. 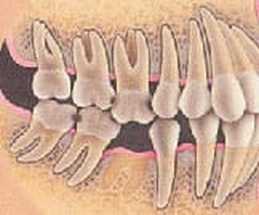 All of this shifting has a domino effect. Since it’s more difficult to clean these areas, cavities develop in the hard to reach areas. Periodontal disease, or so called “gum and bone” disease also develops more easily since you can’t clean these areas. There are solutions for replacing teeth that Dr. Moorhead will cover in a future article. But if you have a choice on whether to save a tooth, you’ll have less cost and a better result if you save your tooth. If you know your teeth need attention, give us a call today! You’ll be glad you did.
Of the three ways you can lose teeth, periodontal disease – also referred to gum disease or gum and bone disease – causes the most tooth loss in adults. Periodontal disease is a silent disease until it reaches advances stages, so without a routine dental exam, you could have it but not know it. Of the half of adult’s that don’t go to the dentist regularly, 80% have serious periodontal disease by age 40. The word “periodontal” describes the structures around that tooth that give it support – the gingival (gums), the bone, and the fibers in-between. Signs that show you may have periodontal disease include:
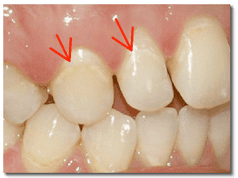
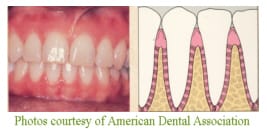
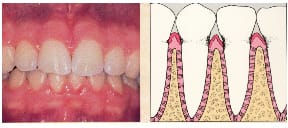
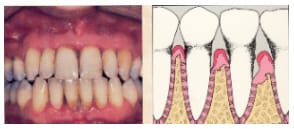
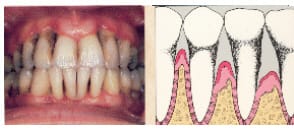
First, let’s take a look at the stages of periodontal disease. This first photo shows an example of healthy gums. The gingival is light pink and flat, and the diagram shows the bone in-between teeth with proper support. Gingivitis is the first stage periodontal disease. Shown in the next photo, gingivitis is a completely reversible disease. The gums are red and swollen, but there is no damage to the bone support. In this third photo, an early stage of periodontitis is shown. You can see the gums pulling away from the teeth as they are losing their bone support. The teeth are sometimes more sensitive where the roots are partially exposed, but often there are no symptoms even at this stage of the disease. Symptoms usually don’t develop until severe bone involvement, so shown here, when the teeth become loose and sore. By this time, it’s often too late to save the involved teeth. To check the health of your gums, your dentist gently slides a measuring probe under your gums. Measurements are made several places around each tooth to show where the gums attach to your tooth, and if there is any bleeding or pus present. If the periodontal support around your tooth is in good shape, the farthest that the probe should be able to measure is 3 mm, or 1/8 inch. This is the farthest that a toothbrush and floss can clean under the gums adequately. A measurement of 4mm or greater demonstrates evidence of periodontal disease. Dentists refer to these areas as “periodontal pockets.” Other signs of periodontal disease include bleeding gums and receding gums.
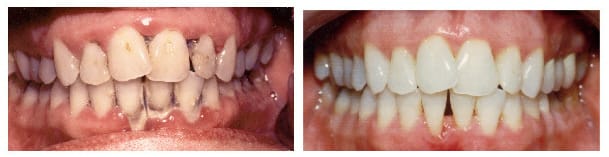
The actual cause of periodontal disease is bacteria that live in these periodontal pockets. In areas this far below the gums, a breeding ground develops for particular types of bacteria called anaerobes, a type of bacteria that thrives where there is no oxygen. These bacteria release toxins that slowly cause destruction of the bone and periodontal fibers that support your teeth. Periodontal disease can be treated if it is caught early enough. Much like a patient with high blood pressure, a patient with periodontal disease cannot be completely “healed” from the damage that has already been caused, but the disease can be controlled so that further damage doesn’t occur. Treatment for periodontal disease will be covered next week. If you’re concerned you may have periodontal disease, why not call us today to schedule an examination. Click here to learn about a special offer for our web readers. You can reach us at Flemingsburg Dental Care at 888-733-3163 As mentioned in the previous article, periodontal disease is the number one cause of tooth loss in adults. Periodontal disease, or so called “gum and bone disease” acts much like termites on the foundation of your house. And like termites, the disease is silent until it is very advanced. Below are photos of one of our patients before and after periodontal treatment. In the left photo, notice the swollen, red gums and the thick tartar on the teeth. When she first came to our office, this patient had periodontal pockets that extended up to 6 mm (1/4”) under the edge of her gums. In addition to improving her appearance, her breath also dramatically improved.
Bacteria thrive in the deep periodontal pockets. The bacteria and its by-products create plaque, and the plaque eventually absorbs calcium from the mouth to form calculus, or in lay terms, tartar. Calculus leaves a very rough surface on the root of the tooth, and even allows the bacteria to imbed itself onto the root surface. Treatment for periodontal disease is primarily aimed at removing the bacteria that cause the disease. One of the primary treatments for periodontal disease is root planing, where the hard deposits of calculus are removed from the root surface, then the root surface is smoothed to remove infected tooth structure. Unlike an ordinary cleaning appointment, root planing is performed in a very detailed fashion under the gums. Root planing can be done comfortably, either by numbing the treated area, or with a product called “Oraqix” that delivers topical anesthetic gel gently into the periodontal pockets to numb the gums without injections. To keep patients even more comfortable, we recommend they take a non-steroidal medication like Advil or Aleve before the root planing, which results in a dramatic decrease in inflammation and discomfort from the procedure. Our office is one of a few in the United States that has ozonated water available to aid in treatment during root planning. In it’s July 2008 edition, the Journal of Contemporary Dental Practice stated that “ozonated water strongly inhibited the formation of dental plaque…(showing that) ozonated water is useful in reducing infections caused by microorganisms present in dental plaque.” Improved home care is also a must in treating periodontal disease. Different tooth brushing techniques are taught to provide additional gentle massage for the infected gums, and daily use of floss or floss substitutes also greatly improve healing. When periodontal pockets are especially deep, a referral to a periodontist, a specialist in gum surgery, may be needed to improve the chances of saving teeth. Because your toothbrush and floss cannot reach further than 3mm (1/8”) below the gums, patients with periodontal disease usually require more frequent cleanings. Only a dental professional can reach these deep areas. By allowing your dental hygienist to perform this gentle cleaning every three months, harmful bacteria are disturbed before they can cause additional damage. If you’re concerned you may have periodontal disease, call us today to schedule an examination. Click here to learn about a special offer for our web readers. You can reach us at Flemingsburg Dental Care at 888-733-3163 |
Articles
All
AuthorDr. Moorhead and his team write about dental news, and answer patient questions. Archives |


 RSS Feed
RSS Feed